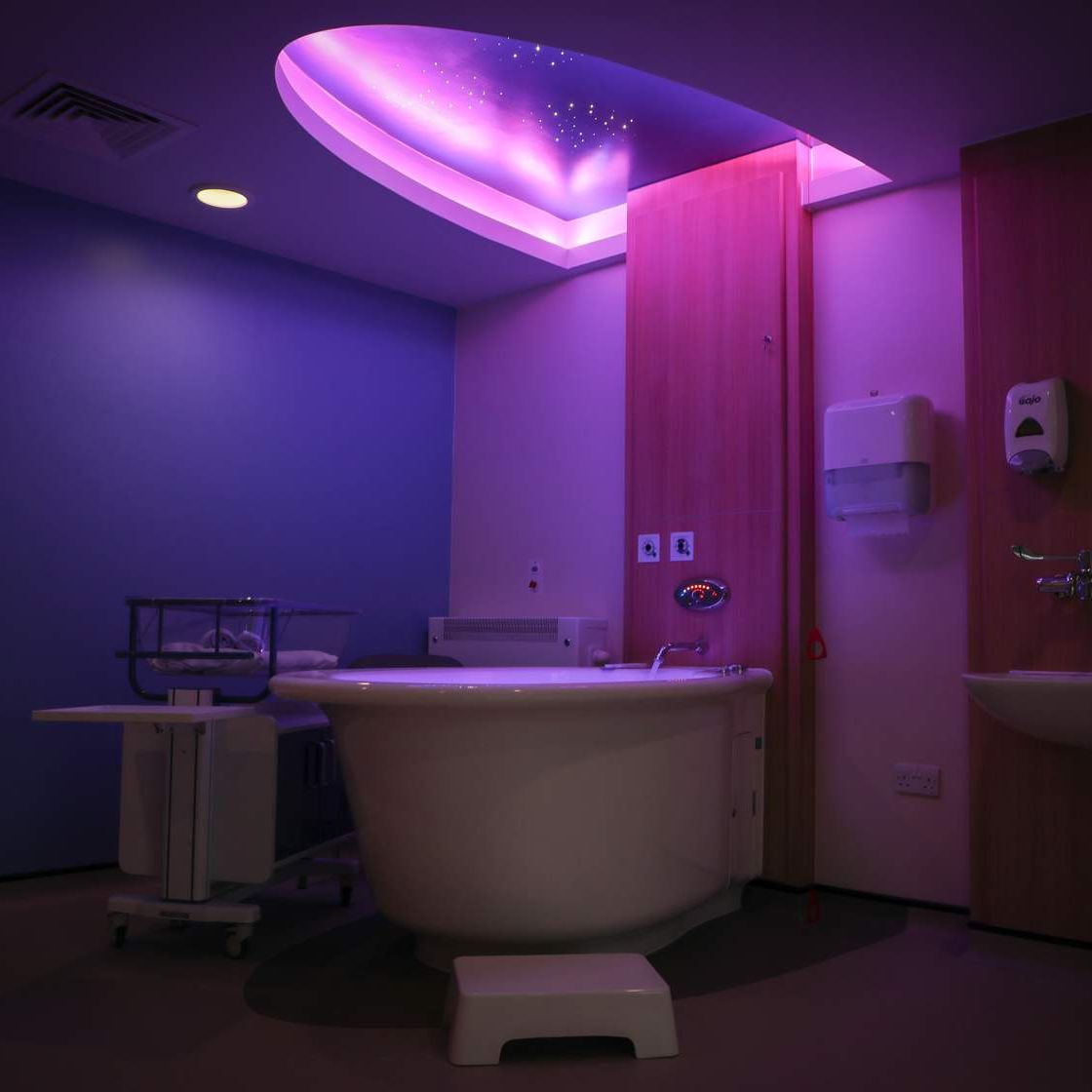
Lancashire Teaching Hospitals aims to provide a range of welcoming, relaxed, comfortable, and supportive environments for you and your family.
We are proud to offer four places of birth:
-
Chorley Birth Centre (Freestanding Birth Centre)
- Preston Birth Centre (Alongside Birth Centre)
- Delivery Suite (Obstetric Unit)
- Home
Childbirth is a major life event and our services are committed to the promotion of a positive life experience, which enhances the long term physical and emotional wellbeing of you and your family.
You and your birth companion(s) are involved in all aspects of care to enable you to make informed choices, feel safe, confident and empowered.
You will be cared for by midwives with the support of maternity support workers, with the help of obstetricians, anaesthetists and neonatologists as required.
All our maternity team provide high quality, evidence-based care, supporting you with competence and confidence.
- Birth Choices - Helping You Decide
- BadgerNet Electronic Health Records at Lancashire Teaching Hospitals
 BadgerNet and Badger Notes -
BadgerNet and Badger Notes -
What is BadgerNet?BadgerNet is a Platform, created and managed by CleverMed Ltd. It is a patient data management service.
BadgerNet Maternity is designed as a full end-to-end maternity system. It allows real-time recording of all events wherever they occur: in the hospital, community, or home. This includes both high risk and low risk pregnancy pathways. Based on a woman-centred care model, the BadgerNet Maternity system comes with a portal for women to view and access their own maternity records online.
 Patient Information for accessing Maternity Notes
Patient Information for accessing Maternity NotesThe Badger Notes App is available from the Apple app store on an iPhone or Google Play on Android phones and allows you to access your maternity records via your smart phone, tablet or PC. This is an “opt-in” service.
The information that appears is generated in real-time from your hospital-based maternity system using details entered by your midwife or other healthcare professionals involved in your care.
BadgerNet can also send emails, text message and push notifications, these will be used to send important health information updates to you during your pregnancy. They will also be used if we need to notify you at short notice of any urgent changes to the service during this challenging period.
Please see Badger Notes (BadgerNotes.net) for a quick rundown of important things you need to know about privacy and your data prior to consenting to use Badger Notes.
You will be able to see the following information:
- Booking Summary
- Antenatal Visits & Future Appointments
- Delivery Summary
- Postnatal Notes
- Summary of Baby’s Care
The app also allows you to:
- Keep a weekly diary and upload photos which you can choose to share with family/friends.
- Access to verified online information and leaflets relevant to your pregnancy.
- Complete your birth plan and share this with your midwife.
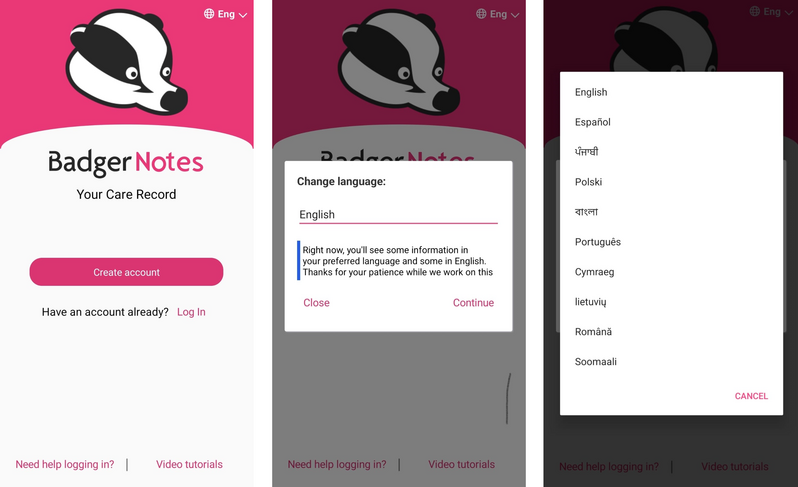
The BadgerNet app can be viewed in ten alternative languages.
Right now, you'll see some information in your preferred language and some in English.
Thanks for your patience whilst BadgerNet work on this.
- Smoking in pregnancy
One of the best things that you can do for your baby is to protect them from tobacco smoke.
Even if you don’t smoke yourself it is important to understand the effects that ‘second hand smoking’ (when people around you smoke) has on both your health and that of your unborn baby.
Did you know…..?
- Every cigarette contains over 4000 chemicals some of which are harmful to your unborn baby.
- Smoking a cigarette reduces the oxygen flow to the baby meaning that their heart has to beat faster every time you smoke.
- Smoking increases the risk of pregnancy complications
- Smoking causes damage to the placenta (afterbirth) which increases the risk of miscarriage, low birth weight, premature birth and stillbirth.
- Smoking increases the risk of cot death
- Second hand smoke also reduces birth weight and increases the risk of cot death.
- Babies whose parents smoke are more likely to be admitted to hospital during their first year of life with lung/breathing conditions.
It is never too late to stop smoking and there is lots of help, advice and support available. During your pregnancy a midwife should discuss smoking with you and offer to refer you to the stop smoking service. At Lancashire Teaching Hospitals, all mums who smoke at the beginning of pregnancy are routinely referred to the stop smoking service.
We advise you to access the specialist advice and support available to help you to quit as this doubles your chances of being successful. You can use nicotine replacement therapy during pregnancy to help you to stop smoking
Carbon monoxide
All women should be offered carbon monoxide screening at the beginning of pregnancy and again at 36 weeks. This is so that the amount of carbon monoxide in your system and the amount passing to your baby can be assessed and advice given.
Carbon monoxide has no colour or smell and is produced when things are burned. It can be found in cigarette smoke, second hand smoke, care exhaust fumes and faulty gas appliances. The test for carbon monoxide is a very simple breath test. If the test results come back high then you should be given advice about reducing the risk of exposure to carbon monoxide. If you don’t smoke and have not been exposed to second hand smoke then you may have a faulty gas appliance and should contact the Health and Safety Executive - gas safety advice line on 0800 300 363
Smoke free homes/Smoke free pregnancy
Lancashire County Council operate a smoke free homes/smoke free pregnancy scheme to reduce the risks of pregnant women, babies and children being exposed to second hand smoke. The smoke free pregnancy scheme can offer referral to your local stop smoking service, arrange for a free home safety visit from the fire service and provide you with some freebies. Ask a midwife or your local children’s centre about signing up to the scheme
Stop smoking advice and support
The following websites may be helpful
www.nhs.uk (NHS choices website)
www.nhs.uk/start4life/stop-smoking
The 'Quit for Us' App can be downloaded free of charge from Google Play and the App Store from the links below:
Apple App Store
https://itunes.apple.com/us/app/quit-for-us/id1039825046?ls=1&mt=8
Google Play Store
https://play.google.com/store/apps/details?id=com.divacreative.quitfortwo
- Feeling your baby move
Movements Matter: feeling your baby move is a sign that they are well

The #movementsmatter campaign, launched by the charity Tommy’s, challenges dangerous myths about baby movement during pregnancy, and tells mums-to-be what to do if they experience a change in their baby's movements. The campaign is supported by NHS England and Kicks Count.
A baby moving during pregnancy can be anything from a flutter, kick, swish or roll and these movements are signs that your baby is well. Most women usually begin to feel their baby move between 16 and 24 weeks of pregnancy.
If your baby is unwell, they may save energy by slowing down their movements.
This can be the first sign of a problem.
Two out of three women who had a stillbirth noticed their baby’s movements had slowed down or stopped.
There is no set number of normal movements. Your baby will have their own pattern of movements that you should get to know. From 16-24 weeks on you should feel the baby move more and more up until 32 weeks, then stay roughly the same until you give birth.
It is not true that babies move less towards the end of pregnancy.
You should continue to feel your baby move right up to the time you go into labour and whilst you are in labour too.
Get to know your baby’s normal pattern of movements.
If you are worried about your baby’s movements do not wait until the next day to seek advice. Contact:
Sharoe Green Unit Triage: 01772 524495
Do not try to make your baby move. If you suspect that movements have slowed, let us know.
Do not use any hand-held monitors, Dopplers or phone apps to check your baby’s heartbeat. Even if you detect a heartbeat, this does not mean your baby is well.
Please watch the video clip and share with your friends and relatives.
There is a leaflet you can download as well: 'Feeling your baby move is a sign that they are well'
Never hesitate to contact us for advice, no matter how many times you are worried about your baby’s movements. We are here to help, 24 hours a day, 7 days a week.
You can find more information about Tommy’s charity via: www.tommys.org
The above leaflet is also available in various other languages:
Albanian: Feeling your baby move is a sigh that they are well in Albanian
Amharic: Feeling your baby move is a sigh that they are well in Amharic
Arabic: Feeling your baby move is a sign that they are well in Arabic
Bengali: Feeling your baby move is a sign that they are well in Bengali
Bulgarian: Feeling your baby move is a sign that they are well in Bulgarian
Chinese: Feeling your baby move is a sign that they are well in Chinese
Farsi: Feeling your baby move is a sigh that they are well in Farsi
French: Feeling your baby move is a sign that they are well in French
German: Feeling your baby move is a sign that they are well in German
Hindi: Feeling your baby move is a sign that they are well in Hindi
Hungarian: Feeling your baby move is a sign that they are well in Hungarian
Indonesian: Feeling your baby move is a sign that they are well in Indonesian
Italian: Feeling your baby move is a sign that they are well in Italian
Kurdish/Somali: Feeling your baby move is a sign that they are well in Kurdish/Somali
Latvian: Feeling your baby move is a sign that they are well in Latvian
Lithuanian: Feeling your baby move is a sign that they are well in Lithuanian
Polish: Feeling your baby move is a sign that they are well in Polish
Portuguese: Feeling your baby move is a sign that they are well in Portuguese
Punjabi: Feeling your baby move is a sign that they are well in Punjabi
Romanian: Feeling your baby move is a sign that they are well in Romanian
Russian: Feeling your baby move is a sign that they are well in Russian
Slovak: Feeling your baby move is a sign that they are well in Slovak
Sorani: Feeling your baby move is a sign that they are well in Sorani
Spanish: Feeling your baby move is a sign that they are well in Spanish
Tigrigna: Feeling your baby move is a sign that they are well in Tigrigna
Turkish: Feeling your baby move is a sign that they are well in Turkish
Urdu: Feeling your baby move is a sign that they are well in Urdu
Vietnamese: Feeling your baby move is a sign that they are well in Vietnamese
- Antenatal
Antenatal services are provided at both Chorley and South Ribble Hospital and Royal Preston Hospital.
The obstetric ultrasound department provides a range of scans including nuchal translucency as part of the first trimester screening for Down’s syndrome, full anatomy scans of the baby between 19-21 weeks gestation as well as growth scans, and other scans as required. Amniocentesis is available to support diagnosis of Down’s syndrome and other chromosomal abnormalities.
Our obstetric consultants each have a specialist interest and we run a range of antenatal clinics :
- Endocrine ANC (e.g. women with thyroid disease) and a joint diabetic/ANC weekly
- Specialist clinic for women with mental health issues
- Multiple births
- Complex and high risk pregnancy
- Premature labour risk
- Obstetric anaesthetics for high risk women
We also provide a range of other services and treatment for pregnant women including :
- Glucose tolerance tests
- Prophylactic Anti D clinics for Rhesus negative women at 28-30 weeks
- Flu clinics (in flu season)
- ECV (external cephalic version) service to massage babies in the breech position to the head presenting position
- Blood tests
Our specialist midwifery team provides additional care for women who may be vulnerable or need extra support including diabetic women, teenagers, women with substance misuse problems, women experiencing domestic violence, women with mental health problems, and when there may be safeguarding issues.
The maternity day unit provides outpatient care seven days a week which you can access directly if you are worried about yourself or your baby, or via referral from your GP or midwife.
- Antenatal Education Course
Antenatal Course
The Real Birth Digital Programme v2.0 is available at Lancashire Teaching Hospitals!
You can now access The Real Birth Digital Programme through your Badger Notes app on the recommended reading section at 26, 30 and 34 weeks or via a QR Code provided by your Midwife.
The programme helps by teaching you more about how your body works in birth and why, helping you to make informed choices which can reduce stress.

- Perinatal Pelvic Health Service (PPHS)
The Perinatal Pelvic Health Physiotherapy Service (PPHS) is a service for pregnant women and birthing people, both during pregnancy and for up to one year following birth, experiencing pelvic health problems such as incontinence or prolapse. We work as part of a wider team with pelvic health midwives, obstetricians and health visitors and we have a role in the perineal clinic.
Visit our Perinatal Pelvic Health Physiotherapy Service (PPHS) page.
- Your Pregnancy Schedule
Your Pregnancy Schedule is pictoral guide to explain when you should attend your antenatal appointments.
You will be offered a range of appointments at locations to suit you and your needs.
If you have complications of pregnancy you may need addtional appointments with one of our team.
- Information Films
Home Birth
Home birth 'Patient Experiences' at Lancashire Teaching Hospitals from Lancashire Teaching Hospitals on Vimeo.
Watch on vimeo Home birth at Lancashire Teaching Hospitals
Skin to Skin
Watch on vimeo Skin to skin at Lancashire Teaching Hospitals
Water in Labour
Watch on vimeo Water in Labour
Tens During Labour
Watch on vimeo Tens During Labour
Pethidine During Labour
Watch on vimeo Pethidine during Labour
Epidurals
Watch on vimeo Epidurals
Entonox in Labour
Watch on vimeo Entonox in Labour
Remifentanil link
Watch on Vimeo
Elective Caesarean Section at Lancashire Teaching Hospitals
Preoperative information for your planned Caesarean
- Latent Labour

- What to do if you think you are in labour
What to do if you think you are in labour
It can sometimes be difficult to decide whether or not you are in labour.
Early signs of labour can occur over several days and may include backache, uncomfortable tightenings (also called Braxton-Hicks contractions), a show or mucousy vaginal loss and needing to use the toilet frequently.
As labour progresses you should begin to notice contractions that become stronger and more frequent. Your waters may break, although the volume of fluid lost varies greatly from one person to another and can sometimes be missed.
You should phone the delivery suite or birth centre to talk to a midwife:
- When your waters break, whether or not you are having contractions
- If you have any fresh red vaginal bleeding
- When your contractions are regular and increasing in strength or when they are approximately 5 minutes apart.
- If you notice that your baby’s movements have reduced
- If you have any concerns. It is not unusual to phone several times for advice and support during the early stages of labour; some women will come in for assessment and then return home until labour is further advanced.
Delivery Suite 01772 524495
Preston Birth Centre 01772 528223
Chorley Birth Centre 01257 245116
Click on the link for more information
https://www.nhs.uk/pregnancy/labour-and-birth
If you are advised to come to the hospital or birth centre, please tell the midwife if you do not have anyone who can bring you. You should not drive if you are in labour.
On arrival, both the Sharoe Green Unit and Chorley Birth Centre have a limited amount of short stay parking near the front door. Birth partners are asked to re-park in the main car parks as soon as possible after escorting you to the delivery suite or birth centre.
At the Sharoe Green Unit, please report to the receptionist on your arrival; the desk is open 8am - 6pm. If the outside doors are locked there is an intercom system to the right of the door.
If you are arriving at Chorley Birth Centre after 5.30pm you will need to use the door bell and intercom at the main maternity unit door (not the antenatal clinic entrance) to let the midwives know you have arrived. Before 5.30pm, you can make your own way up to the Birth Centre on the second floor. Please use the intercom if you need any assistance.
- Vaginal Birth after Caesarean
For most women pregnancy and birth are healthy normal life events. For a number of reasons some births may result in a caesarean section.
If you have had a caesarean section you may be thinking of how you may birth this time. Vaginal birth after caesarean (VBAC) is a term used for women who birth vaginally after having had a caesarean birth in the past.
If you have had a baby by caesarean it does not necessarily mean that any babies you have in the future will also be born in this way.
We have a team at Lancashire Teaching Hospitals who can provide you with support and information. This will allow you to make your own informed birth choices. Planning a VBAC or choosing an elective repeat caesarean section has different risks and benefits.
In considering your options, your previous pregnancies and medical history are important factors to take into consideration.
You will be seen in the birth after caesarean clinic, between 16-25 weeks of pregnancy. The clinic is held on delivery suite and gives you the option to view a birth room and surrounding environment. You are more than welcome to bring your birth partner. A referral will be made for you at your booking appointment, by your midwife; if feel you need to speak to one of the team members sooner then please email vbacclinic@lthtr.nhs.uk
During your clinic appointment you will have the chance to talk about your previous experiences of birth and labour, giving us the opportunity to plan your forthcoming birth.
You do not need to make a decision at this appointment, however, we work closely with a team of obstetricians and if we feel a referral needs to be made to a consultant obstetrician or you would like to discuss this further this can be done on the same day.
For more information please click here
- Elective Caesarean Section
- Skin to Skin
- Safer Sleep
Videos
Here are 6 videos covering different scenarios when the normal sleep routine is interrupted. For example, when the family is on holiday or parents have had a night out.
Click the image below to view the videos or watch here https://vimeo.com/showcase/8571682
The Named Midwife and Public Health Midwife at Lancashire Teaching Hospitals in conjunction with the Safeguarding Midwives across the Local Maternity System (LMS) have led on the production of these six videos.
- ICON

ICON is an evidence based programme which provides a simple message that supports parents/care givers to cope with infant crying.
Most people who have ever cared for a baby appreciate some advice about how to comfort a crying baby and how to cope when it goes on for a long time.
Our Public Health specialist midwife and Safeguarding Lead midwife have made an informative video, see link below for the video and the ICON webpage.
- Tongue-tie (Frenulotomy) service
Visible Lingual Frenulum (Tongue Tie)
Beneath the tongue is a piece of skin which attaches the front of the tongue to the floor of the mouth. This is called the lingual frenulum (lingual means tongue). In some new born babies the frenulum can be abnormally short and restrictive to the movement of the tongue—known as a Tongue Tie. This means the tongue does not move up and forward as it would with a normal frenulum.
Many visible frenulum’s’ do not cause any problems at all and do not need to be treated
What problems can tongue tie cause?
A restricted frenulum – otherwise known as a tongue tie, may cause problems with breast feeding and less often bottle feeding. The problems caused by tongue tie during breastfeeding are due to trouble with latching. Latching is the name given for the connection between the baby’s mouth and the mother’s breast.
Problems for the mother
- Sore, cracked nipples
- Mastitis (painful, swollen breasts)
- Poor latch
- Short, frequent or longer feeds. This can be exhausting for the mother.
- Frustration and a sense of failure with breastfeeding
Problems for the baby
- Difficulty in staying on the breast or bottle during feeding
- Slow to gain enough weight
- Leaking milk from side of mouth whilst sucking
- Clicking during feeding
- Colic and wind (caused by the baby swallowing air during feeds).
My baby is feeding well but has a visible frenulum:
If your baby is feeding well, tongue-tie division is not considered necessary; as your baby grows the tongue-tie may stretch or naturally divide. However, it is important to reconsider dividing your baby’s tongue tie if the transfer of food from the front to the back of the mouth and ability to chew properly appears to be affected when you introduce solid foods. Tongue tie division may then be indicated clinically; however older babies will require a light general anaesthetic, as they are less likely to remain still during the procedure.
Whilst the majority of children who have a frenulum under their tongue that is not divided have no difficulties with their speech, the presence of a tongue tie has been shown to influence the ability to pronounce certain sounds in some children. However, it is not possible to predict which children will be affected, or to determine whether intervention as a baby will prevent this. Some babies that have tongue tie division still go on to need further intervention as a child. This will normally be noticeable when your baby reaches three years of age and may necessitate referral to a speech and language therapist, who will advise you as to whether or not division of the tongue tie under a general anaesthetic will be of benefit.
Where can I have my baby’s tongue tie released?
If you are having problems feeding your baby and suspect there is a tongue tie you can contact your GP, midwife or health visitor. If there are no feeding issues, we cannot offer the procedure at this Trust. They will know how to refer you to our local assessment service within our local Lancashire Teaching Hospitals NHS Foundation Trust.
During this appointment, your baby’s mouth and tongue will be assessed for suitability of releasing the Tongue Tie. Releasing the Tongue Tie may not be appropriate if the assessment identifies adequate tongue movement which shows the frenulum does not restrict the tongue. In this case the specialist will suggest other ways in which we can help you with your feeding concerns.
How long will it take to get an appointment in Tongue Tie Clinic?
Once a referral has been sent you will be contacted regarding an appointment within 7 working days. Please be advised that in periods of high demand, priority for appointments will be made on clinical need.
What happens at the clinic appointment?
During the appointment, your baby’s mouth and tongue will be assessed for suitability of releasing the Tongue Tie. Releasing the Tongue Tie may not be appropriate if the assessment identifies adequate tongue movement which shows the frenulum does not restrict the tongue. In this case the specialist will suggest other ways in which we can help you with your feeding concerns. If after assessing your baby’s mouth and tongue tie, it is deemed as suitable for division, the practitioner will discuss the procedure and gain your written consent.
The procedure does not need a general anaesthetic or local anaesthetic. It is not appropriate to give a local anaesthetic because the frenulum has a poor blood and nerve supply. All risks and benefits will be discussed during the consultation.
We ask that you are able to feed your baby following the procedure, and may also require an observation of a feed during the consultation.
Further Information
Our service can assess babies in our midwife led outpatient clinic up to the age of 12 weeks at the time of the appointment and live within Central Lancashire.
For further information, please contact our Infant Feeding Specialist Midwife on 01772 524512 or via email at: tonguetieclinic@lthtr.nhs.uk